Sepsis Prevention
Developed as a collaborative effort involving Nursing and Physician staff/leadership and Quality and Safety experts, the update to the Sepsis Prevention Program launched on September 26th, 2017. As a leading cause of in-hospital mortality, early recognition and action are the most important concepts in achieving the best possible outcome for our patients.
The most important part of sepsis treatment is getting the 3 hour bundle elements completed within the three hours following start of Time Zero. Here at Piedmont, we have a screening process through EPIC that helps us identify patients that have worsening sepsis. Similar to code blue, code red, etc. we have a code sepsis. This screening process begins with the patients primary nurse.
activation of code sepsis
what the primary nurse will see on patients who meet screening criteria
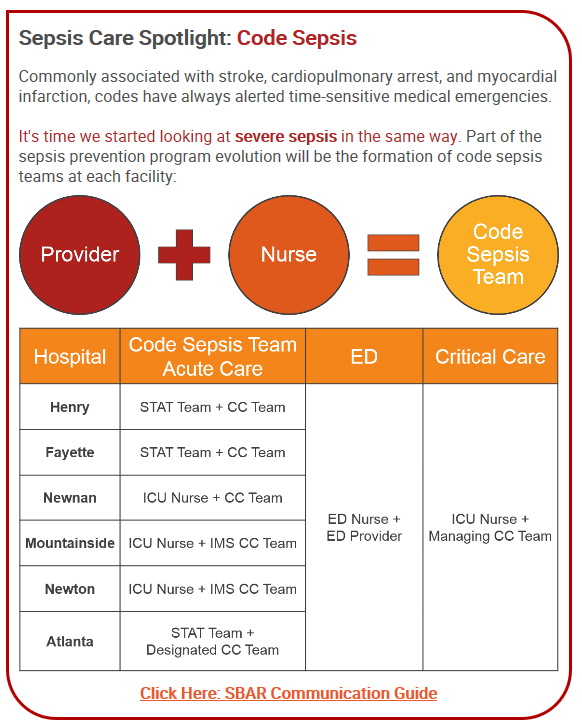
the code sepsis team for each hospital
In the inpatient setting, the patients primary nurse will be asked - Is the patient showing signs and symptoms of a new or worsening infection?
If the answer is YES and the patient has >/= 2 clinical criterias of infection, >/= 1 clinical criteria of organ dysfunction, then the code sepsis (red) BPA will fire on EPIC.
This activates the code sepsis team, which is different at each hospital. The stat team or ICU nurse will go and evaluate the patient; once evaluated, they will call the critical care APP. This is time zero.
The member of the critical care team (MD/APP) who evaluates the patient will then do a sepsis rule in/rule out.
BPA DOTPHRASE WALKTHROUGH
The Sepsis Order set Tracker
Once a patient is bundled for sepsis, they should be added to the sepsis order set tracker. This can only be done in the nursing screen; it is on the nursing sepsis narrator (“0—> 3 hour bundle start”). Once initiated, in order to see the tracker, do the following steps:
Step 1
Step One: Click your hospital on the bottom left of the EPIC screen.
Step 2
Step two: Under your hospital, click “sepsis management”.
Step 3
Step three: when you click sepsis management, this will pop up below it.
Step 4
the sepsis tracker will pop up. If you do not see a patient here they have not been added to the sepsis tracker list. Here you will see what components of the bundle have been completed.